We are currently upgrading our website. Please bear with us if you are experiencing any loading issues.

APACMed
The Voice of MedTech in Asia
Virtual Event

9 June | 3:00pm – 6:30pm SGT
Remote Care Management
The Future of Patient Care Symposium
APACMed presents the second instalment of Digital Health Symposium, under a continued theme of Remote Care Management (RCM).
This year, The Future of Patient Care Symposium is structured around the Remote Care Management user experience: healthcare professionals, patients/caregivers, and wider society. Thought leaders from across the region and globe will convene to outline the remaining gaps, share best practices, and exchange real life stories on topics ranging from Remote Care Management use, value demonstration to reimbursement to economic sustainability.
Elisabeth Staudinger
Board Sponsor of APACMed Digital Health Committee &
Managing Board Member and Head of Asia Pacific, Siemens Healthineers
What is Remote Care Management?
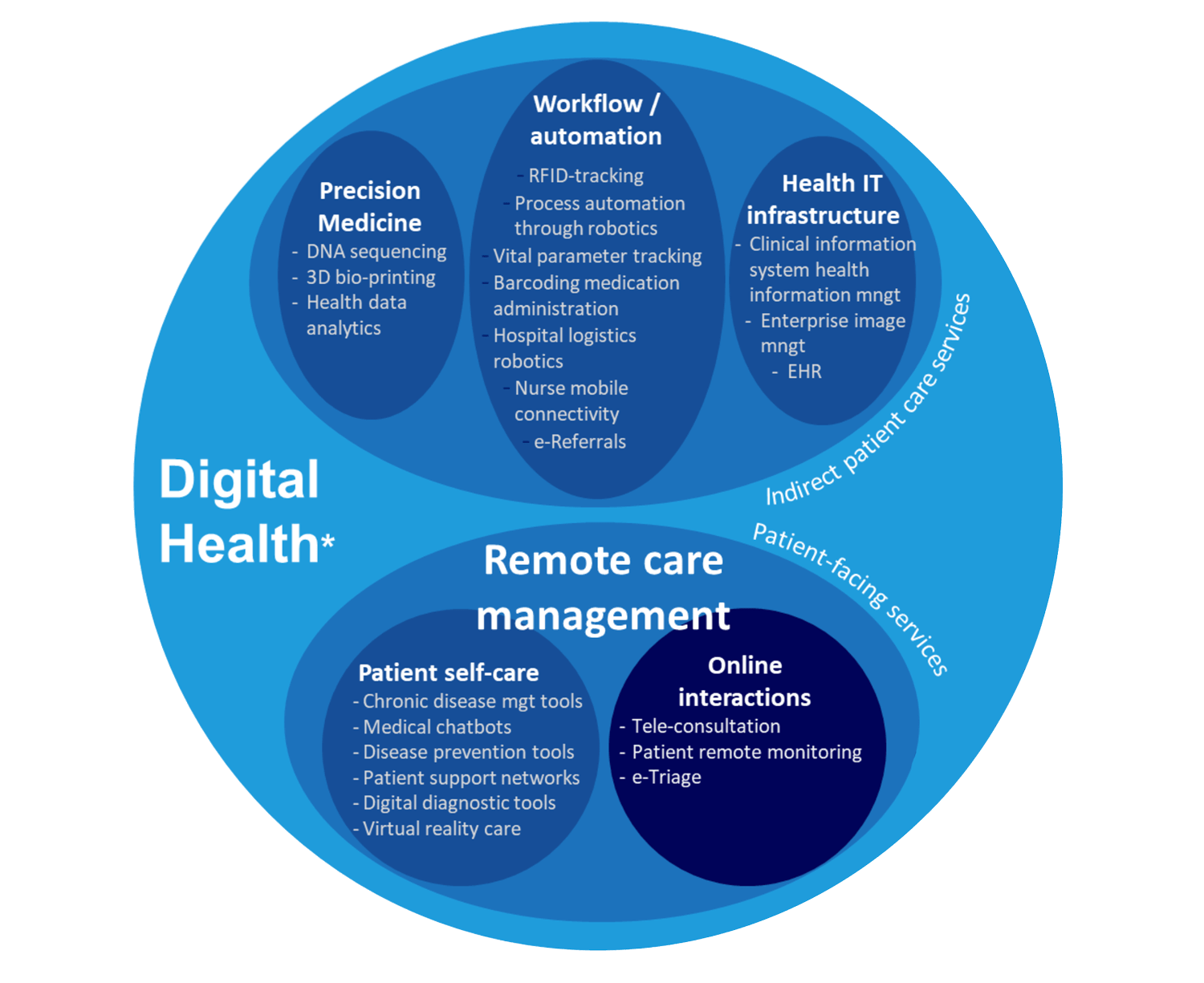
Remote Care Management (RCM) encompasses patient-facing digital technologies and services as a means to facilitate clinically driven remote monitoring, care and education of patients. As has been demonstrated during COVID-19, Remote Care Management is a necessity for care providers, payers and governments striving to implement an effective population health management strategy.
Remote Care Management initiatives must enable patient pathways outside of conventional clinical settings, such as in the home or in rural geographies, thereby increasing access to care and decreasing delivery expenditures. As indicated by the diagram, Remote Care Management initiatives typically come in one of two solution categories – online patient interactions and patient self-care.
“Digital Health Symposium 2021 was a phenomenal opportunity for us to kickstart the hot topic of RCM in the Asia Pacific. In 2022, the intention is to take the topic even further, by exploring the viewpoints of other ecosystem stakeholders and continuing to share best practices about what works in driving appropriate Remote Care Management adoption.”

Andrew Frye
Chair of APACMed Board and President of Baxter Asia Pacific
While certainly we’ve made great progress on the Remote Care Management topic, due to COVID-19, there remain many hurdles ahead to capturing the desired health, social, and economic outcomes. It is key for us to continue to understand various stakeholders’ perspectives; please consider doing your part by joining to contribute to the conversation.

Elisabeth Staudinger
Chair of APACMed Digital Health Committee and President of Siemens Healthineers Asia Pacific
Symposium Challenge Statements
The Future of Patient Care Symposium seeks to address a few key challenge statements:
- How can healthcare professionals and care providers work better, thanks to Remote Care Management?
- What is still not working for patients, despite the promises?
- What value does Remote Care Management deliver to the wider healthcare ecosystem and society?
Bearing these challenge statements in mind, the Symposium agenda contains three distinct Remote Care Management segments below:
The Healthcare Professional and Provider Experience
A master-class style use case format, we go deep in providing a platform for peer exchange. In particular, we will look at how Remote Care Management enables collaboration across silos, with the shared ambition of better management of patients along the entire journey of multiple disease state interventions.
The Patient Experience
Through real life stories shared, we will highlight what is working as well as where the issues in adoption remain. Human centricity remains a key focus for Remote Care Management, hence discussions will be held on critical enablers such as patient empowerment, digital health literacy and data privacy.
The Wider Society Experience
Payment incentives remain the main driver of Remote Care Management adoption. Measuring the value of this new way to deliver care becomes crucial, but the appropriate methodology is still missing. Beyond the clinical and financial potential of Remote Care Management, we must also consider the impact on quality and productivity of life, driven by improvement in healthcare outcomes from Remote Care Management. At the same time, the funding models of Remote Care Management must be sustainable for society too.
Join the conversation at The Future of Patient Care Symposium, to help shape the adoption of Remote Care Management solutions in Asia Pacific. Connect with peers across public and private sector, in the healthcare industry and beyond.
Who Should Attend?
- leaders from pharma/medtech/digital health corporate companies
- healthcare providers, healthcare professionals
- payers
- academia
- tech firms
- governments
- policymakers
- start-ups
- patient groups, and more
The Future of Patient Care Symposium Agenda
Time in SGT (+8 GMT)
Opening & Keynote Address
3:00 — 3:15pm SGT
Welcome by APACMed
Keynote Address

Roberta Sarno
Head of Digital Health, APACMed

A/Prof Low Cheng Ooi
Chief Technology Officer, Sheares Healthcare Management Pte. Ltd.; Senior Advisor, CMIO Office, Ministry of Health Singapore
The Healthcare Professional and Provider Experience
3:15 — 4:00pm SGT
A look through the lens of Health Care Professionals and Providers at how Remote Care Management enables collaboration across silos, with the shared ambition of better management of patients along the entire journey of multiple disease state interventions.

Chris Jia
Vice President, Digital Growth, United Family Healthcare

Anne Betzner
Vice President of Programs and Evaluation,
Children’s HeartLink

Mengwei Xin (Moderator)
Partner, Leader, Health Systems and Services Practice (China & Asia), McKinsey & Company
The Patient Experience
4:00 — 4:45pm SGT
Human centricity remains a key focus for Remote Care Management, hence we go further downstream to discuss from the Patient’s viewpoint: what critical enablers are working and conversely, what still does not work despite promises?

Birgit Bauer
Social Media & Digital Health Expert, Journalist, Speaker & Analyst, Patient Expert, Manufaktur für Antworten UG

Tanya Hall
CEO and Founder, hearts4heart

Yoann Sapanel (Moderator)
Head, Health Innovation, WisDM, Institute for Digital Medicine, NUS School of Medicine
Coffee Break
4:45 — 5:15pm SGT
The Wider Society Experience
5:15 — 6:00pm SGT
We demonstrate the value of the digital health for the ecosystem including Healthcare professionals, providers, patients, caregivers, society. This discussion will emphasize how value is delivered and measured, across stakeholder categories, into the Remote Care Management future.

Dr William Gordon, MD, MBI, FAMIA
Assistant Professor of Medicine, Harvard Medical School; Associate Physician, Brigham & Women’s Hospital

Dr Izzuna Mudla Mohamed Ghazali
Public Health Physician/ Deputy Director, Medical Development Division, Ministry of Health Malaysia; Head, Malaysian Health Technology Assessment Section (MaHTAS)

Arif Fahim (Moderator)
APACMed Chair of Digital Health Reimbursement; Regional Director – Asia Pacific, Global Health Economics & Reimbursement, Abbott Medical Devices
Conclusion
6:00 — 6:30pm SGT
Keynote Address: A look ahead on Remote Care Management in Asia Pacific
Closing Remarks

Farhana Nakooda
General Manager & Senior Vice President, Health Catalyst

Roberta Sarno
Head of Digital Health, APACMed
Meet Our Speakers

A/Prof Low Cheng Ooi
Chief Technology Officer, Sheares Healthcare Management Pte. Ltd.; Senior Advisor, CMIO Office, Ministry of Health Singapore
Read Bio
A/Prof Low Cheng Ooi
A/Prof Low Cheng Ooi is an orthopaedic surgeon by training. During his 8 year tenure as Chief Medical Informatics Officer at Ministry of Health, he had the opportunity to use and develop analytics to help gain insights in order to improve care clinically and nationally. He joined Sheares Healthcare Group as Chief Technology Officer in September 2020 and continues to serve as Senior Advisor in the CMIO’s office at Ministry of Health, Singapore.

Chris Jia
Vice President, Digital Growth, United Family Healthcare
Read Bio
Chris Jia
Bio coming soon.

Anne Betzner
Vice President of Programs and Evaluation Children’s HeartLink
Read Bio
Anne Betzner
Anne Betzner, Ph.D., oversees program development and standardization, program impact measurement, quality improvement and research efforts at Children’s HeartLink (CHL). She oversees CHL’s 18 partnerships across five countries and likes working with systems and using stories and hard statistics to improve performance for social betterment. Before joining CHL Anne served as senior research scientist at Allina Health and was Vice President at Professional Data Analysts, Inc., a research and evaluation consulting firm. Anne has a master’s degree in policy analysis and a doctorate in research methods from the University of Minnesota. Anne loves serving her community through volunteering with The Minnesota International NGO Network, The Humphrey School of Public Affairs Alumni Board, The University of Minnesota Alumni Association Collegiate Council and her church.

Mengwei Xin
Partner, Leader, Health Systems and Services Practice (China & Asia), McKinsey & Company
Read Bio
Mengwei Xin
Bio coming soon.

Birgit Bauer
Social Media & Digital Health Expert, Journalist, Speaker & Analyst, Patient Expert, Manufaktur für Antworten UG
Read Bio
Birgit Bauer
Birgit Bauer, Social Media & Digital Health Expert, Journalist, Speaker and Analyst and Patient Expert
Birgit is German and works with a Business Partner in the company, the Manufaktur für Antworten UG (www.manufaktur-fuer-antworten.de) . Birgit works as Social Media and Digital Health Expert, Journalist and Speaker with a more than 17 years’ experience and a specialisation in Healthcare, developing Workshops and Talks about the use of Social Media for Target Groups e.g. Patients, Patient Organisation, NPO, Industry and BioTech Companies, Start-Ups and governmental institutions. In her role as Consultant, she designs and realize Social Media – and Communication Strategies for different Businesses or Patient Projects and brings the Ideas and Strategies into the reality. With a team Birgit also designs and performs Feasibility Studies.
Birgit aka @Birgitpower on Twitter (https://twitter.com/Birgitpower) is one of the most influential Blogger about Multiple Sclerosis and Healthcare in Germany and Europe. She started her Blog “Fast normal! Mein Leben mit MS” – “Almost normal – My Life with MS” http://leben-arbeiten-mit-multiple-sklerose.blogspot.de/ in 2007.
Birgit is a so-called Patient Expert and Eupati Fellow. She supports the European Multiple Sclerosis Platform voluntary, is a proud member of the Editorial Board of the “Data Saves Lives” Initiative, is HIMSSFuture50 Patient Leader 2021 and Member of the Stakeholder Group of the Tehdas Project. Birgit is also involved in different Advisory Boards, Committees and Focus Groups. She is a Co-Author of different scientific Whitepapers and Publications around the theme “Patient – Doctor Communication”.
Birgit about Digital Health Solutions:
“Digital Health Solutions can help people living with chronic conditions in different ways. There are a lot of benefits for patients in the digital world to make lives easier. And we have to find the best ways how to use those tools in a meaningful way and explain this to the patients and citizens to make sure, that everyone is on board of the digital train. Because digital health is not an enemy, it can be a great assistant for us all to make lives easier, grow quality of life and help doctors to have more quality time with the patient.”

Tanya Hall
CEO and Founder, hearts4heart
Read Bio
Tanya Hall
Tanya has contributed over 10 years work within the not-for-profit sector. She is a passionate leader with strong networks and a track record of delivery across the community and health industries.
As CEO of the only cardiac patient advocacy group actively involved in market access discussions with Government, Tanya has been successful in re-energising the Australian cardiac community in the patient access to therapies discussion. She has also united Industry companies through roundtable meetings and regular conferences, to bring a single voice to the issue. Tanya has also made significant contributions through her involvement with the Parliamentary Committees of ‘Friends of Heart & Stroke’ & ‘Friends of Medicine’.
Early detection and patient access to therapies across the globe is Tanya’s goal. Tanya’s passion to both raise awareness of heart disease and ensure patients have treatment and access to proven therapies, has seen her establish relationships with key stakeholders including clinicians, politicians and health industry members.
Tanya represents consumers on several key committees including the Therapeutic Goods Administration (TGA) Device Reform committee, ECG review committee, ANZCETS Committee, Cardiac Society of Australia and New Zealand Australasian Cardiac Procedures Outcomes Registry, Cardiac Society of Australia and New Zealand Australasian Cardiac Device Outcomes Registry, AF Ablation percutaneous catheter ablation writing committee, Global Heart Hub Heart Valve and Heart Failure Committees, Continuity of Care Collaboration Committee. CEO Tanya Hall is also a co- author of the Australian Clinical Guidelines for Atrial Fibrillation.

Yoann Sapanel
Head, Health Innovation, WisDM, Institute for Digital Medicine, NUS School of Medicine
Read Bio
Yoann Sapanel
Yoann is Head of Health Innovation at WisDM, the Institute for Digital Medicine at the NUS School of Medicine. With the team, he aims to foster and accelerate cross-industry, public–private collaborations to validate, implement and scale first-of-its-kind pharmacological and digital interventional technology into the clinic. Prior to that, Yoann was the health of Health Partnerships at MetLife Asia’s innovation center, focusing on the development of new products and services grounded in technology and data for cancer, dementia and cardiovascular diseases. During his time at Medtronic, Yoann was leading the APAC CoE for Business Model Innovation, which aimed to address the inefficiencies across the care continuum with innovative solutions. As the program director for Medtronic Asia’s Value Based Health Care Council, Yoann was also instrumental in advancing the acceleration and adoption of outcome-based models to ensure better patients outcomes, reduce costs, and deliver value across the Region.

Dr William Gordon, MD, MBI, FAMIA
Assistant Professor of Medicine, Harvard Medical School; Associate Physician, Brigham & Women’s Hospital
Read Bio
William Gordon, MD, MBI, FAMIA
William Gordon, MD, MBI, FAMIA is an internist and clinical informaticist at Brigham and Women’s Hospital and Mass General Brigham in Boston, Massachusetts.
Dr. Gordon has spent more than a decade working in healthcare information technology, and has written extensively on information security, interoperability, data standards, and digital product development.
He is currently faculty in the Division of General Internal Medicine and Primary Care at Brigham and Women’s Hospital, the Department of Biomedical Informatics at Harvard Medical School, and he is the Director of Solution and Experience for Digital Care Transformation at Mass General Brigham, where he leads a product management team tasked with building virtual care programs.
Dr. Gordon is an attending physician in the hospital medicine unit at Brigham and Women’s Hospital and an Assistant Professor of Medicine at Harvard Medical School.

Dr Izzuna Mudla Mohamed Ghazali
Public Health Physician/ Deputy Director, Medical Development Division, Ministry of Health Malaysia; Head, Malaysian Health Technology Assessment Section (MaHTAS)
Read Bio
Dr. Izzuna Mudla Mohamed Ghazali
Dr. Izzuna Mudla Mohamed Ghazali is the Deputy Director of the Medical Development Division, Ministry of Health Malaysia, and the Head of the Malaysian Health Technology Assessment Section (MaHTAS). She is a Public Health Physician and joined MaHTAS in 2007. Since then, she has conducted reviews on various types of health technologies. She also play a key role in planning and implementation of health technology assessment, development, and implementation of clinical practice guidelines, and was the responsible person to set up horizon scanning of emerging health technologies activity for the Ministry of Health Malaysia. She was the Head of Horizon Scanning, Communication, and Information Unit at MaHTAS from 2013 until 2020. Dr. Izzuna is actively involved at the local and international levels. She is a visiting lecturer at the University of Malaya, University of Science Malaysia, and Cyberjaya University. She is also a member of various committees at the national level including Cluster of Emerging Technologies, Nutritional Research, National Technology Innovation Sandbox, and National Rare Disease Committee. At the international level, she is currently the Vice President of HTAsiaLink, Regional Coordinator for AsiaScan, the regional group for the Asia Pacific Region of the International Health TechScan (i-HTS), and a member of the organizing committee for HTAi Asia Policy Forum. She has also published articles on public health matters and health technology assessment.

Arif Fahim
APACMed Chair of Digital Health Reimbursement; Regional Director – Asia Pacific, Global Health Economics & Reimbursement, Abbott Medical Devices
Read Bio
Arif Fahim
Arif Fahim is part of Abbott’s APAC Regional Leadership team for the Medical Devices Division. He holds overall functional responsibilities for the Health Economics & Reimbursement (HE&R) shared service across business portfolios of Cardiac Rhythm Management (CRM), Electrophysiology, Heart Failure, Vascular, Structural Heart, and Neuromodulation. In addition, Arif also currently Chairs the Global Task Force on Early Value Assessment at Abbott.
In his current role, Arif leads a team of HE&R country managers across all major geographies in the region including Japan, China, India, Australia/New Zealand, Southeast Asia, Taiwan and South Korea. He has extensive experience in driving commercial and cross-functional partnerships, implementing innovative out-of-the-box approaches to market access, providing industry thought leadership, and driving multi-country, regional and global projects.
He has successfully negotiated numerous market access/entry agreements/premium requests with Governments and commercial health insurers across the region, which entails working closely with healthcare payers and HTA agencies, developing value-based solutions for medical devices procurement/adoption, building new business models and market intelligence based support systems, and fostering cross industry partnerships.
Arif is an active member of the Market Access WG and the Digital Health Reimbursement WG at APACMED, the HTAi Asia Policy forum, and formerly at AdvaMed, where he served as Vice Chair of the India WG and Chair of the Health Economics, Pricing and Reimbursement Sub-group.
Arif has attended Executive education at INSEAD and Yale School of Management, trained in HTA and Health Economics, including advance methods in cost effectiveness analysis and outcomes measurement, from the Centre of Health Economics, University of York, UK, and is an academic awardee and Masters’ Degree holder in Marketing and Strategy from the University of Durham, UK.

Farhana Nakhooda
General Manager & Senior Vice President, Health Catalyst
Read Bio
Farhana Nakhooda
Farhana Nakhooda, GM & SVP Health Catalyst, Asia Pacific, leads the overall vision and growth strategy of the Health Catalyst business across Asia Pacific. She is passionate about improving healthcare outcomes, access to care as well as decreasing healthcare costs across the APAC region. She has extensive experience with engagement at the intersection of medicine, technology, AI and analytics. Prior to joining Health Catalyst, Farhana was the IBM Healthcare & Life Sciences solutions leader for Asia Pacific for 18 years where she played a key role in digitally enabling healthcare transformation projects across Asia Pacific, Eastern Europe and Middle East/Africa. She has more than 25 years of international experience in the healthcare and life sciences industry as a medical researcher and as a subject matter expert. Farhana has a Bachelor of Science degree (with Honors), in which she majored in Biology and Biochemistry, at the University of British Columbia. She completed her MBA at Monash Mt Eliza Business School in Melbourne, Australia.

Roberta Sarno
Manger, Digital Health, APACMed
Read Bio
Roberta Sarno
Roberta joined APACMed in December 2019 to lead the new Digital Health Committee. She supports the association’s members to establish a digital health ecosystem, build knowledge and advocate for optimal policies that help digital health innovation in APAC.
Prior to joining APACMed, Roberta worked as senior consultant and business development manager at Alcimed in Paris and Marseille, France, where she supported clients in the healthcare sector on innovation and strategy projects. Before that, she worked as genetic engineering researcher at Curie Institute, in collaboration with the French startup Meiogenix.
She holds a PhD in genetics (Curie Institute, Paris), a master of business foundations (INSEAD) and lives in Singapore.
Ticket Price

27 June 2022
from SG$
00
*Registration is required for free Virtual Ticket for APACMed members.
Other Symposiums
Thank you to our Sponsors and Partners
At ResMed we pioneer innovative solutions that treat and keep people out of the hospital, empowering them to live healthier, higher-quality lives. Our digital health technologies and cloud-connected medical devices transform care for people with sleep apnea, COPD, and other chronic diseases. Our comprehensive out-of-hospital software platforms support the professionals and caregivers who help people stay healthy in the home or care setting of their choice. By enabling better care, we improve quality of life, reduce the impact of chronic disease, and lower costs for consumers and healthcare systems in more than 140 countries.
Roche established a presence in the Asia Pacific in 1925. Today, we operate in 16 locations across the Asia Pacific region from Pakistan to Australia and New Zealand, supported by more than 5,700 employees. With the industry’s most comprehensive diagnostics portfolio, we are committed to innovate diagnostics, shaping healthcare and changing lives. Roche is a leader in research-focused healthcare with combined strengths in pharmaceuticals and diagnostics. Roche is the world’s largest biotech company, with truly differentiated medicines in oncology, immunology, infectious diseases, ophthalmology and neuroscience.
Siemens Healthineeers constantly brings breakthrough innovations to market, helping healthcare professionals deliver high-quality care, leading to the best possible outcome for patients. Patient-centered innovation has been and always will be at the core of Siemens Healthineers. They aspire to create better outcomes and experiences for patients from all geographies.
Sponsors receive the exclusive opportunity to physically attend the Symposiums at our event venue.
For sponsorship opportunities, please contact Gabriel Sim.
Knowledge Partner
BROUGHT TO YOU BY

HELD IN